These organisms have a range of mechanisms to prevent the action of many antimicrobials used in clinical medicine. Sulfamethoxazole-trimethoprim remains the mainstay of treatment. 
These mechanisms, associated or separate, restrict the treatment options to an alarming level. 
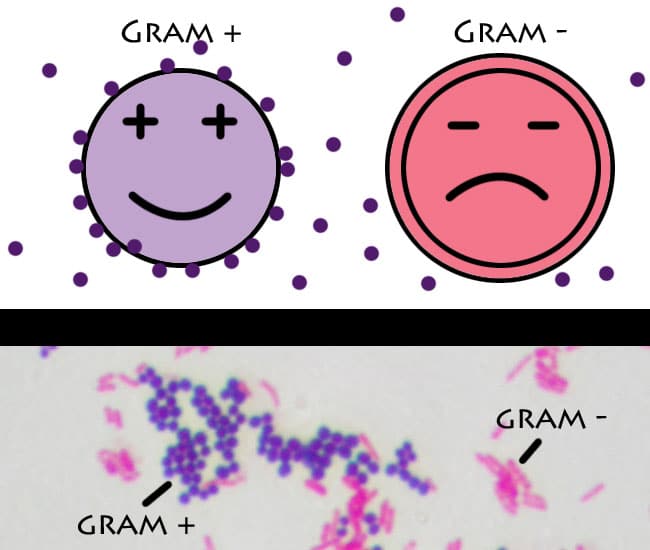
Thus, Stenotrophomonas present several efflux pumps and produce two carbapenemases – L1 (resistance to all carbapenems) and L2 (cephalosporinase). The Stenotrophomonas exhibit a pattern of intrinsic multi-resistance, especially in patients who have had contact with carbapenems. The genetic ingenuity of this microorganism goes further, and it combines high impermeability with genetic plasticity, combining with the resistance of mechanisms such as extended-spectrum b-lactamases (ESBL). The most frequent are MexAB-OprM and loss of OprD (which gives impermeability to the bacterial cell due to the loss of porin.) Acinetobacter baumannii naturally produces AmpC cephalosporinase and oxacillinase (OXA), leaving it spontaneously immune to many drugs. aeruginosa, cephalosporinase of type AmpC, and efflux systems that confer resistance to b-lactams. The critical issue regarding BNF, when it comes to the antimicrobial sensitivity profile, is undoubtedly their intrinsic resistance since they produce a variety of genes with multiple mechanisms capable of mitigating the microbicidal action. The main BNF microorganisms that cause human disease are Pseudomonas aeruginosa, Acinetobacter baumannii, Burkholderia cepacia, Burkholderia pseudomallei, Stenotrophomonas., Alcaligenes, and Moraxella. These stand out for being aerobic and non-sporulated they are incapable of fermenting sugars, using them through the oxidative route. They also cause opportunistic diseases in ICU patients who undergo invasive procedures. The non-fermenter, gram-negative bacilli (BNF) have a lower frequency of isolation when compared to Enterobacteriaceae however, they are a relevant group since they cause severe, fatal infections, especially in the hospital environment. Laboratory characterization is an essential component when it comes to microorganisms therefore, it is imperative to expose characteristics of Enterobacteriaceae, which are bacilli, non-sporulated, have variable motility, grow in the presence and absence of oxygen, ferment organisms of glucose, are cytochrome oxidase negative, and can reduce nitrate to nitrite. The general/species that frequently affect humans are Escherichia, Proteus, Enterobacter, Klebsiella, Citrobacter, Yersinia, Shigella, and Salmonella, among others. They account for about 80% of gram-negative isolates with a myriad of disease-causing general/species in humans, including urinary tract infections, pneumonia, diarrhea, meningitis, sepsis, endotoxic shock, and many others. Two large groups, Enterobacteriaceae and the non-fermenters, are responsible for most clinical isolates nevertheless, other clinically concerning gram-negative organisms exist, including but not limited to Neisseria, Haemophilus spp., Helicobacter pylori, and Chlamydia trachomatis.Įnterobacteriaceae are a heterogeneous group widely dispersed in nature. These microorganisms have significant clinical importance in hospitals because they put patients in the intensive care unit (ICU) at high risk and lead to high morbidity and mortality. Overall, the toxins produced by Gram-negative bacteria can cause many symptoms and complications, and treatment typically involves antibiotics and supportive care for any related symptoms or complications.Gram-negative bacteria (GNB) are among the world's most significant public health problems due to their high resistance to antibiotics. LPS can contribute to sepsis and other conditions associated with Gram-negative bacterial infections. Lipopolysaccharides (LPS) are also part of the cell wall of Gram-negative bacteria and can stimulate the immune system to produce inflammation and other responses.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
